-
- Face-Body
- Dermatology
- Plastic Surgery
- Hair Loss
- HOT Treatments
- About us
- Career Opportunities
- Contact
Face
- Botox
- Brotox
- Hyaluronic Acid Fillers
- Facial Thread Lift
- HIFU Face
- Fractional Laser CO2
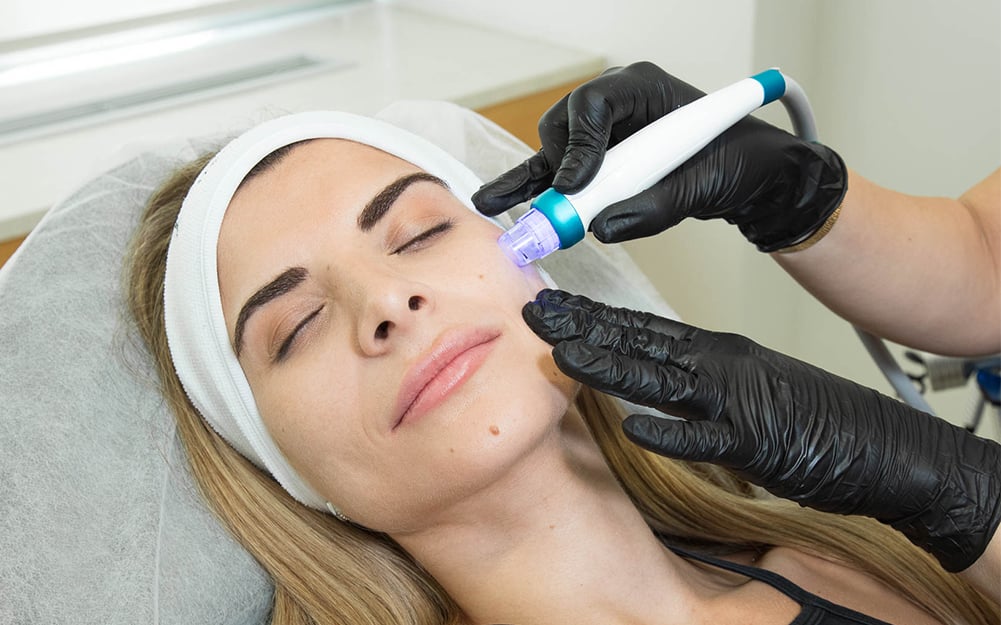
- Microneedling
- Facial Mesotherapy
- Profhilo Skin Booster
- Eye Booster
- PRP – Facial Autologous Mesotherapy
- Total Plasma Lift
- Glowlift
- Ultrasound RF
- Hydrabeauty
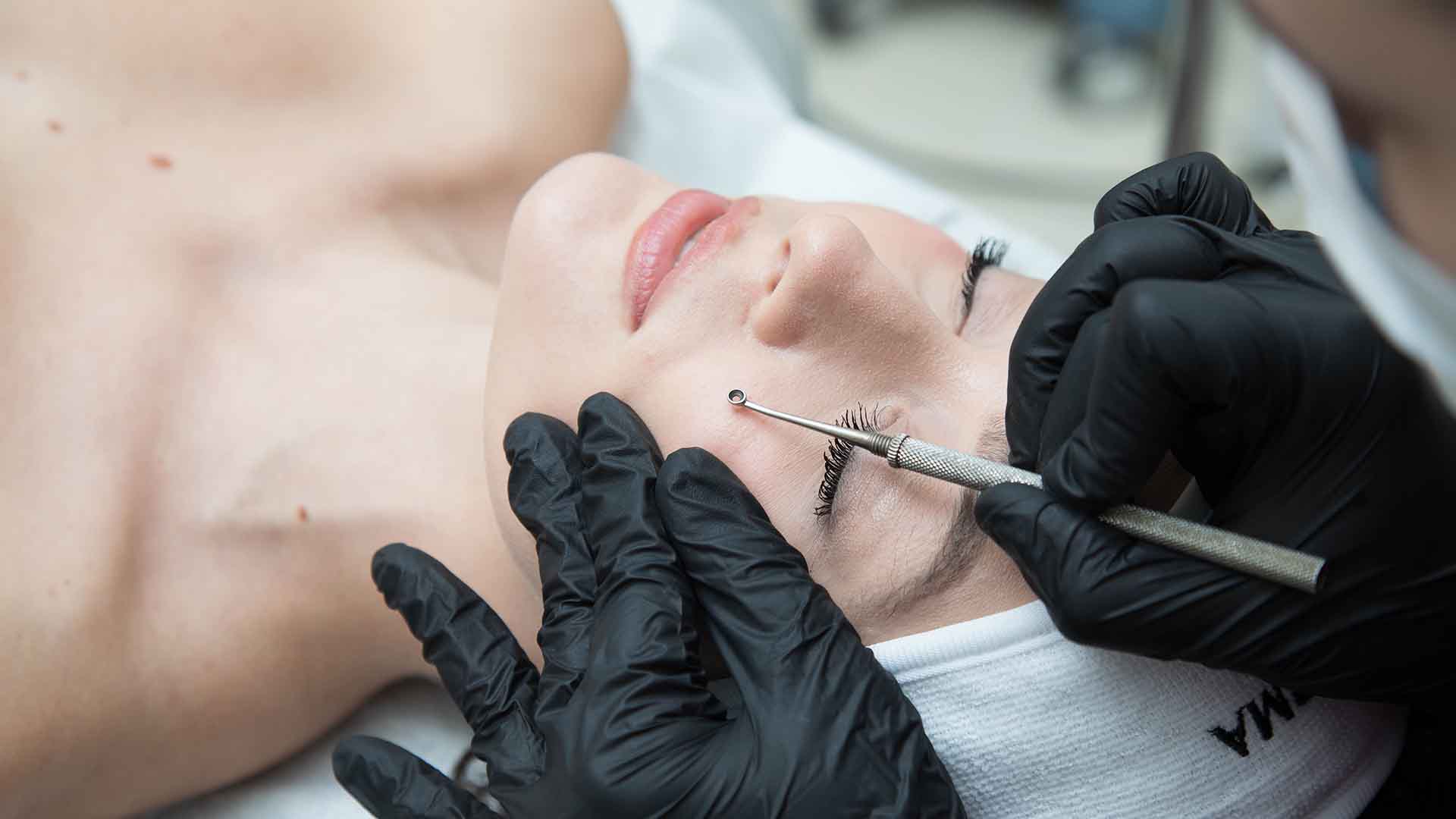
- Facial Cleansing
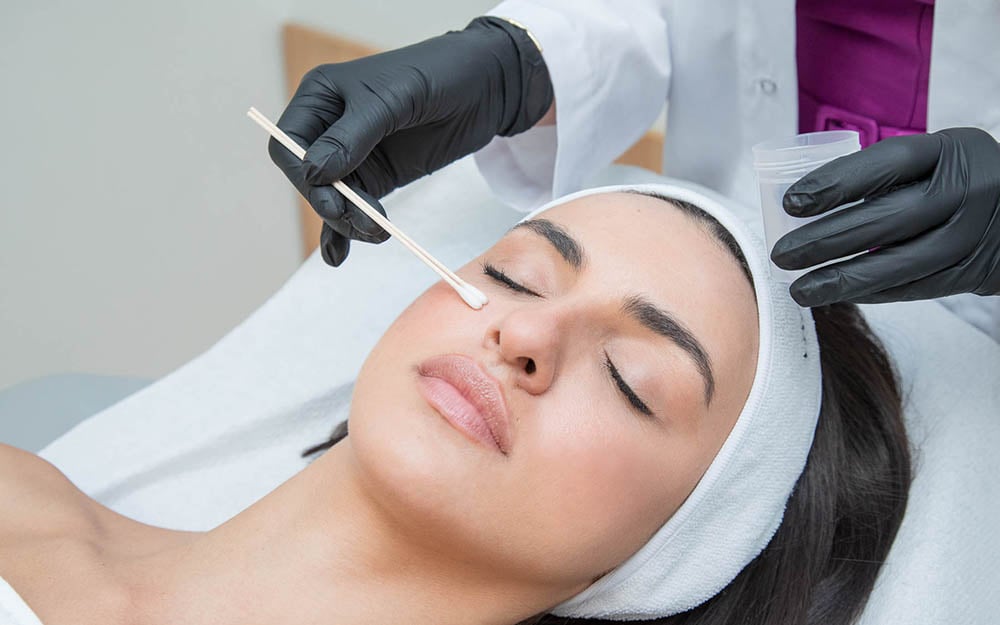
- Chemical Peeling
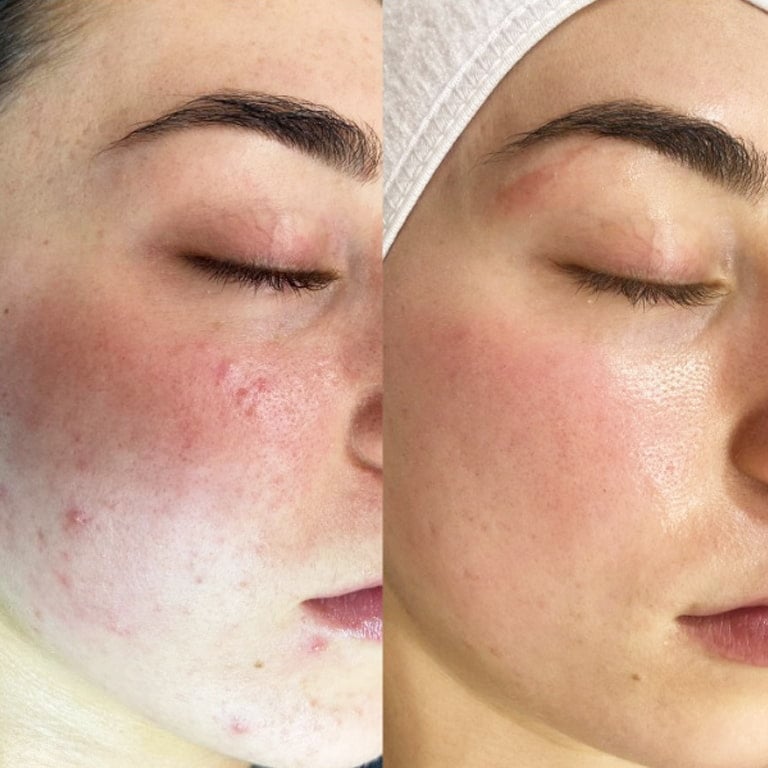
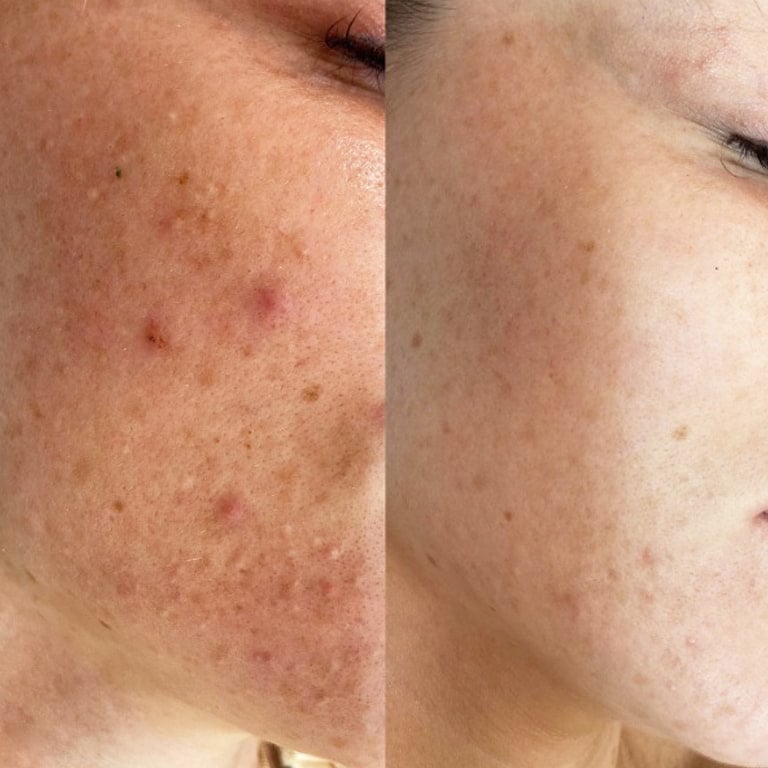
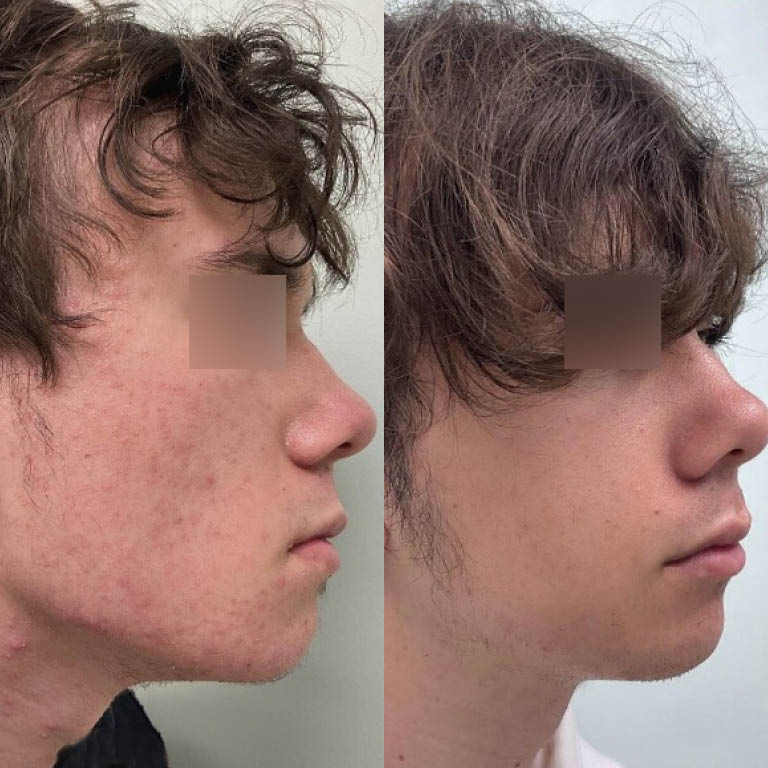
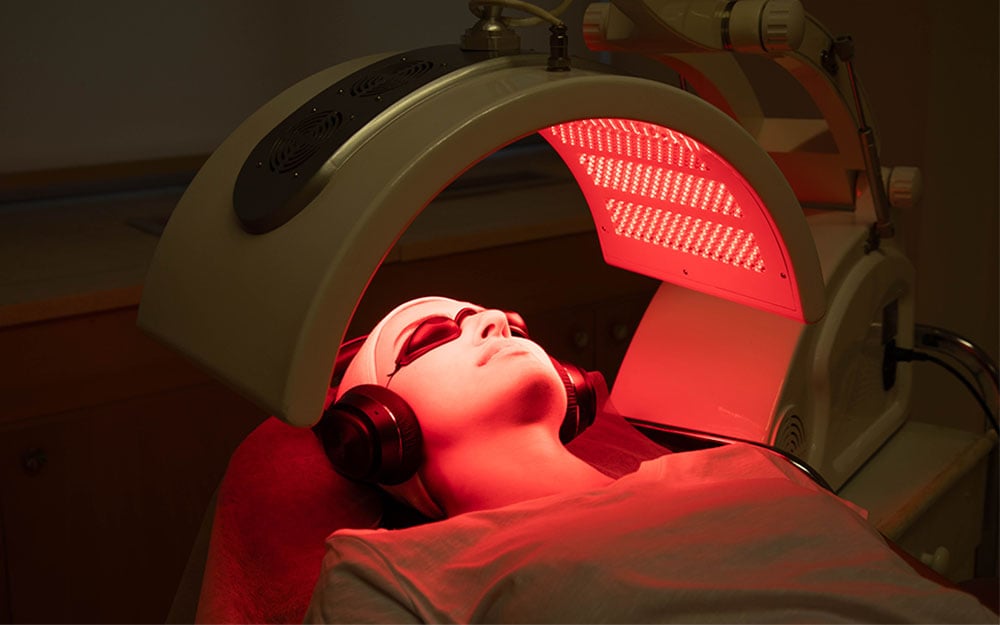
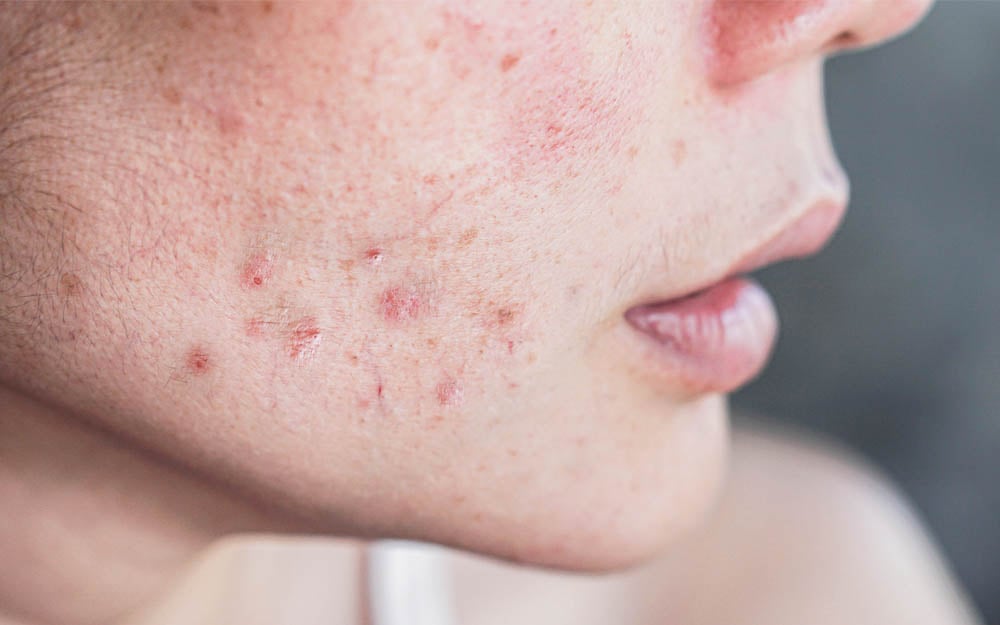
- PDT Photodynamic Acne Treatment
- Skin Analyzer
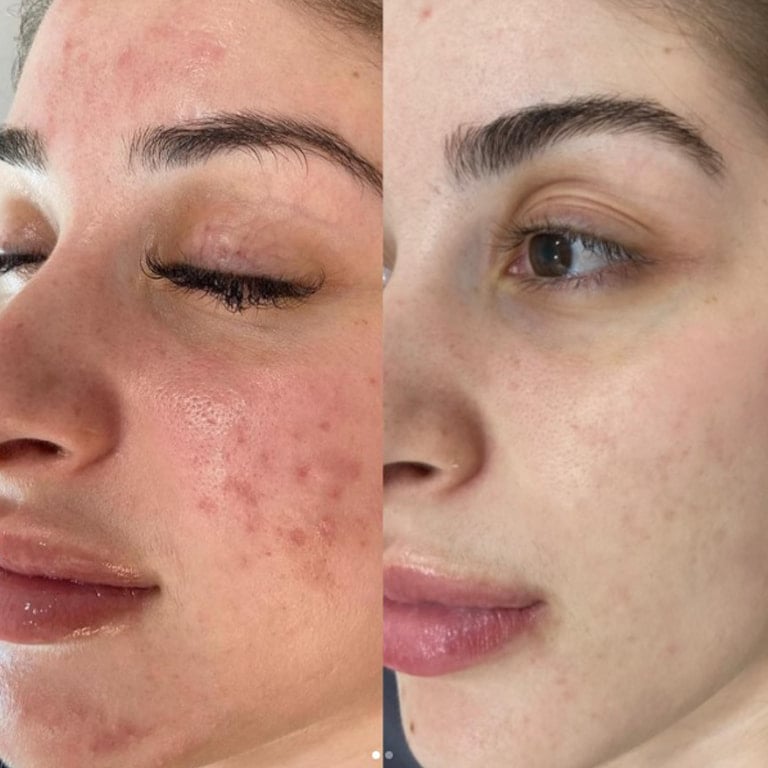
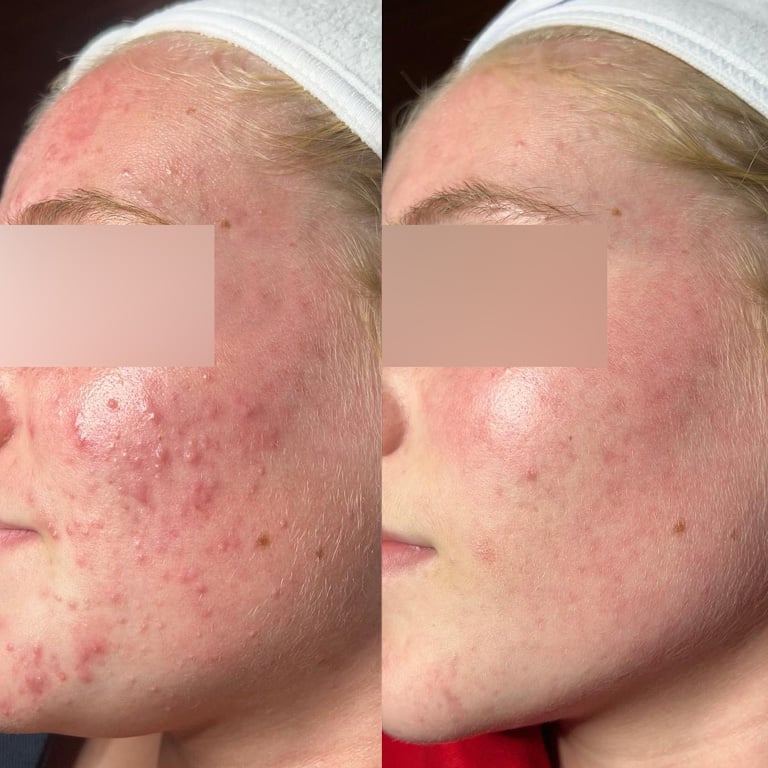
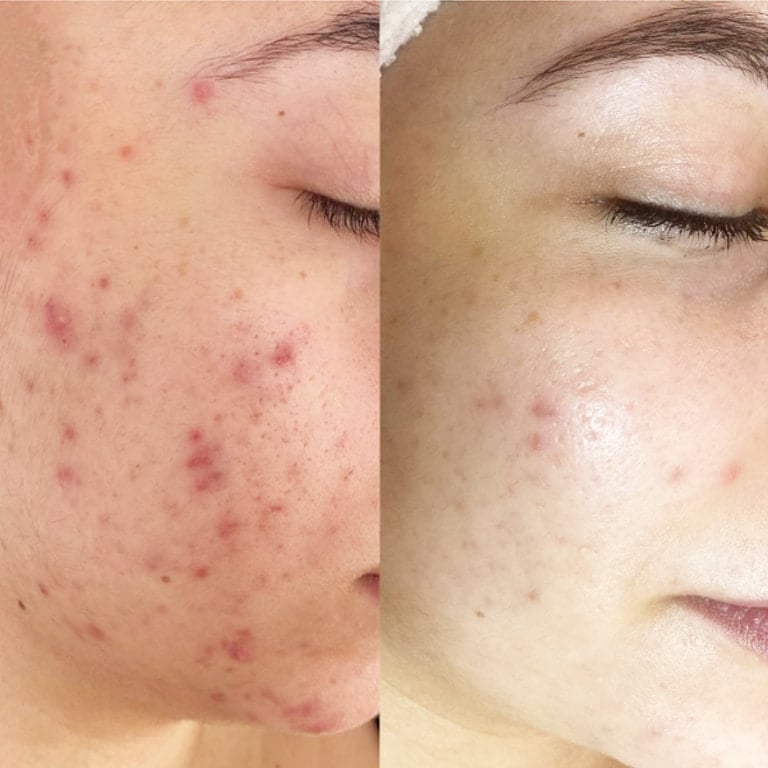
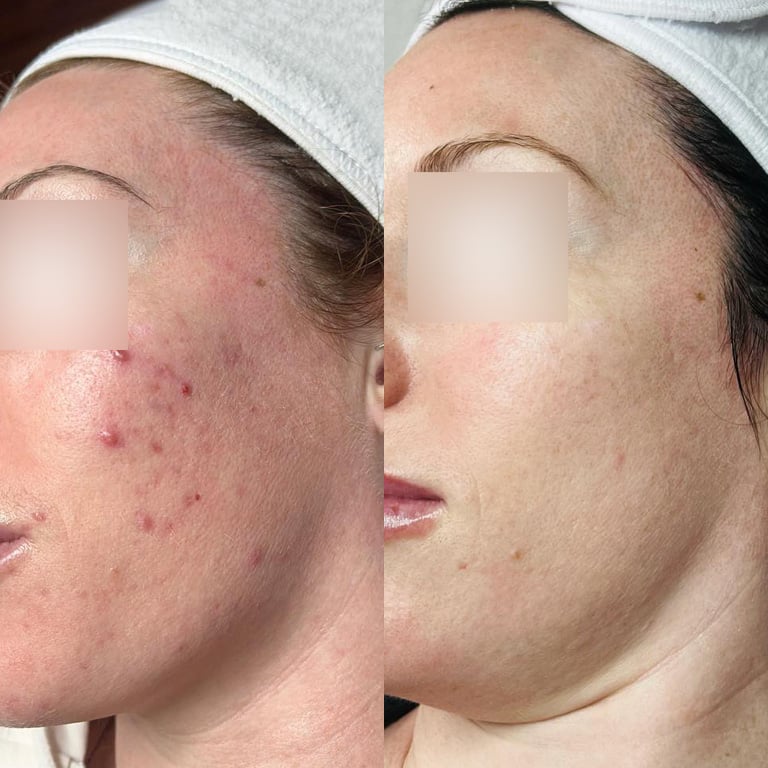
- Acne Scars
- Spider Veins Treatment
- Lentigines – Liver Spots
- Bloodless Rhinoplasty
- Laser Hair Removal
Plastic Surgery
Tab 5 Content
The Group
Cosmetic Derma Medicine is today the largest and most reliable unit of Aesthetic & Clinical Dermatology and Plastic Surgery, with 15 state-of-the-art Clinics in Greece and Cyprus
Medical Team
The specialized dermatologists and plastic surgeons of our clinic, together with an experienced medical team of various specialties, offer solutions to clinical problems of skin diseases and aesthetic medicine issues.
Contact Form
The specialized medical team, the modern medical methods and the modern and luxurious spaces of the clinics offer the ultimate experience of hospitality, service and provision of health and beauty services.
Contact Information
Athens
Working Hours
Monday-Friday: 09:00-20:00
Saturday: 09:00-18:00
Our other clinics